Majority of operating rooms are not ergonomically friendly for the healthcare workers, particularly during lateral patient transfer. This leads to various prolonged musculoskeletal disorders. This prevailing issue is a threat to staff retention and healthcare staff. Moreover, it threatens safe patient transfer and operational throughput.
The Anatomy of Injuries in operating room for healthcare workers
The operating room presents a unique ergonomic paradox. In a high velocity environment, the surgical team executes lateral transfer of patients, approximately 20 times. These patient transfers are biomechanically distant from other handling tasks. Some of the common factors that lead to musculoskeletal disorders in healthcare workers during a lateral transfer are,
The Dead Weight Factor
In the operating room, the patients are often premedicated, anesthetized or are recovering from the anesthesia. The patients in this state lack the muscle tone to assist in the lateral transfer. Consequently, this ultimately leads to the healthcare workers bearing up to 100% of the patient transport load.
Spinal Stress Caused by Extended Reaching during Patient Transfer
The mobility of the healthcare workers in the operating room is limited during patient transfer due to the presence of sterile areas, IV poles, anesthesia machines and robotic equipment. This equipment makes the staff reach farther than normal. This extended reaching puts strain on the spine. For example, even reaching just 20 inches puts on extra pressure on the back by up to ten times.
Patient Transport – A Rush to Save Turnover time (TOT)
Healthcare workers are often rushed to reduce turnover time. This can lead to compromising on their health and bypassing safety protocols of standard number of staff mandatory during patient transport. A meta-analysis of work-related musculoskeletal disorders among nurses found an annual prevalence of 77.2%. The breakdown of affected anatomical areas shows the prevalence of lower back pain to be 60%, neck pain to be 53% and shoulder pain to be 47%.
These statistics highlight the urgent need for mechanical interventions. The old methods of manual lifting using a draw sheet and calling for count of three is biomechanically indefensible in modern ergonomic science.
The High Cost of Manual Patient Transport
The direct and indirect costs associated with musculoskeletal disorders in the health care industry is estimated to be $20 billion annually. The direct cost includes medical treatments, indemnity payments and workers compensation. Whereas the indirect cost includes staff turnover and lost productivity. It also includes hospitals facing legal liability for failing to provide adequate equipment to protect their healthcare workers from any injuries. Moreover, for hospitals to replace a specialized operating room nurse can cost around $60,000 to $100,000 in recruitment and training expenses.
In this context, the SurgyLift emerges as a tool for healthcare workers and patient safety. It not only helps in risk management but saves the healthcare facilities from financial setbacks.
SurgyLift: A revolutionary solution for Patient Transport
SurgyLift is a patient lift system that utilizes a specialized inflatable mattress system to bear the weight of the patient during lateral transfer.

Zero Friction Lateral Transfer with SurgyLift
SurgyLift is a mechanical patient transport system that protects the spine of the healthcare worker. It does so by effectively reducing the friction coefficient to zero during lateral transfers.
The SurgyLift bridge Functionality
SurgyLift patient transferring system is placed below the patient and assists the staff with safely transferring them from one surface to another. The SurgyLift acts as a bridge between the two beds, providing patient safety and ergonomic support to the operating room staff.
Securing patient transport with SurgyLift Stability
The body strap in the SurgyLift provides stability, ensuring the patient is secure during the transfer. This stability is crucial in the operating room. In this environment, a fall would be catastrophic.
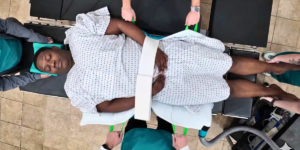
Optimizing Bariatric Patient Transport with the SurgyLift
SurgyLift allows high volume OTs to easily schedule bariatric cases, as it can handle 400 lb patients with the same speed and staffing requirement as 150 lb patients.
SurgyLift: A Safer Alternative to Sling-Based Patient lifts
Lateral patient transfer protects the surgical patients with incisions, lines or fractures, unlike sling lifts that tend to scrunch the patient, causing a halt to patient safety.
Mitigating Shoulder and Neck Injuries
During patient transfers the reaching and pulling movement creates a high torque on the glenohumeral joint. This often leads to rotator cuff tears. SurgyLift solves that problem by eliminating forceful traction. The OR staff merely guides the device by keeping their elbows close to their bodies and maintaining a power position, thereby preserving should and neck integrity.
Extending Careers with SurgyLift Patient Transport
SurgyLift extends the careers of the older more experienced OR staff by protecting them from musculoskeletal disorders. It acts as a force multiplier, allowing older staff to manage heavy patients with reduced risk.
Creating a safe climate with SurgyLift
A study conducted by NIOSH indicated the safe patient handling programs and initiatives that creates an ergonomically safe environment for the healthcare workers, led to nursing personnel indicating their backs were less sore and they were less tired at the end of the shift. This psychological shift happened because they were less stressed during patient transfer not worrying about any ergonomic injury.
Eliminate the Manual lifting injuries and optimize staff retention by reducing risk associated with patient transfers. Book a demo for SurgyLift today.




