The skill of the surgeon in laparoscopic surgery is often determined by the time a patient takes in recovery. This recovery is based on a major unspoken variable that determines the results long after the surgery is done and it is the microscopic purity of the surgeon’s instruments. The emerging research supports the transition to single-use laparoscopic instruments for patient safety and hospital solvency.
The Anatomy of an Invisible Threat
One of the most expensive and prevalent healthcare related infections are surgical site infections. While the chances of infection in laparoscopic surgery is minimal, the presence of pathogens into a sterile cavity by contaminated surgical instruments leads to deep incisional or organ space surgical site infections.
The danger of reusable laparoscopic instruments lies in their inherent complexity. These surgical instruments often feature:
- Blind Spots: A laparoscopic scissor or a set of graspers/dissectors in surgery consists of long shaft with narrow lumens and recessed hinges.
- The Sterilization Paradox: These blind spot areas are notorious for trapping bioburden, such as blood and tissue, which can survive the high heat of an autoclave.
- Residual Debris: Studies confirm that even “clean” instruments often carry residual protein, acting as a direct vector for cross-contamination.
Precision and Clinical Outcomes
Beyond sterility, the mechanical condition of a laparoscopic scissor plays a direct role in infection risk.
- Tissue Trauma: Reusable scissors lose edge integrity after as few as 5–10 uses. Dull blades lead to tissue crushing and tearing rather than a clean cut.
- Healing Complications: Unlike the atraumatic separation provided by single use laparoscopic instruments, tissue trauma from dull reusable tools increases the risk of postoperative leaks and opportunistic infections.
The Staggering Financial Burden of SSIs
While the unit price of single use laparoscopic instruments is often higher than a single “use cycle” of a reusable tool, the financial analysis changes drastically when SSIs are factored in.
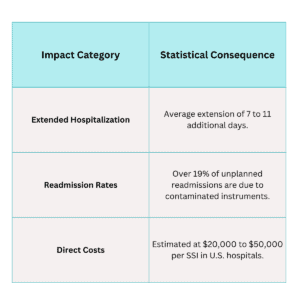
The CMS Penalty Factor (2026 Update)
As of 2026, the Centers for Medicare & Medicaid Services (CMS) has intensified its “Hospital-Acquired Condition (HAC) Reduction Program”. Hospitals ranking in the worst-performing quartile for infection rates face a 1% reduction in all Medicare payments. For a large facility, this penalty far exceeds the cost of switching to disposable inventory.
The Disposable Solution: A Strategic Transition
Investing in high-quality single use laparoscopic instruments provides a closed-loop sterility assurance model.
- Guaranteed Sterility: Factory-sterilized tools like the laparoscopic scissor or lap aspiration needle ensure precision and eliminate any possibility of cross-patient contamination.
- Advanced Electrosurgery: Disposable electrodes avoid insulation breakage frequently seen in reusable laparoscopic instruments, which can result in unintended thermal damage.
- Fluid Control: Modern tools like the lap aspiration needle now include transparent shafts to allow maximum visibility and avoid internal contamination.
- Reliable Grasping: Specialized forceps in surgery provide consistent mechanical performance without the risk of “pitting” seen in older steel.
By choosing to eliminate the $25,000 risk of an SSI and protecting your facility from CMS penalties, you provide your surgical team with the highest quality surgeons instruments on the market.